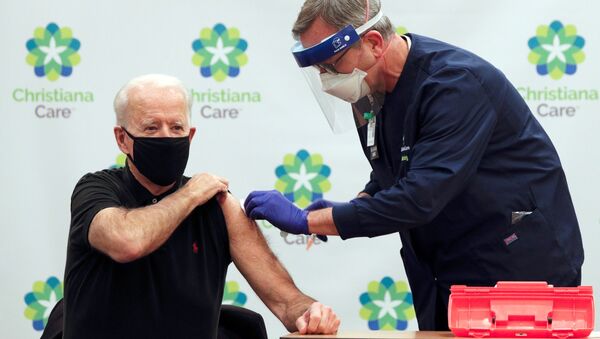
One of the first executive orders the new US president signed on his first day in office was an array of measures directed at stopping the deadly march of the coronavirus pandemic in the country, which has already claimed the lives of more than 400,000 Americans. One of the provisions of the president's decree ordered "coordinating the Federal Government’s efforts to support the timely, safe, and effective delivery of COVID-19 vaccines".
Indeed, with two vaccines authorised in December and the vaccination campaign kicking off on 14 December, the US administered only 24.6 million shots with only a little above 3.8 million out of 328 million Americans getting the full two-shot immunity by 27 January, according to CDC data. It was clear from the start that the newly developed vaccine will not be available in large enough quantities to inoculate the entire country at the start, and it remains one of the key obstacles to giving shots to more people in the US, according to Ana Santos Rutschman, assistant professor of Law at Saint Louis University.

Numerous American states and cities have faced a lack of new supplies of the vaccines. New York reported cancelled some 23,000 appointments for shots because of a shortage after a delay in Moderna vaccine deliveries was announced. Miami, San Francisco and West Virginia reported similar problems. Frisco said it got a fraction of earlier weekly vaccine supplies this week.
The critics of the previous administration blamed the hiccup on the policy of Trump's cabinet, often placing hopes on the new administration of Joe Biden to fix the issue. However, the data, potentially explaining the reason so few people got the shots, suggests that several factors contributed to the issue and it is unclear how many of them the Democrat administration will be able to fix.
Local Authorities Partly to Blame?
The CDC data shows that production rates were not the only bottleneck that hindered mass vaccination efforts in the country. Some 47.2 million dozes of vaccines have so far been distributed across all the states since the start of the vaccination drive, but only 24.6 million dozes have been administered. The reason for this huge discrepancy lies in poor articulation of plans to distribute and administer vaccines at the local level, which resulted in some shots of medicine going to waste, Rutschman explains. Though the states are following some general guidelines provided by the CDC - for example, who should be inoculated first - each local authority still goes by its own vaccination plans, she says.
Indeed, some of the states fared significantly better than others in using vaccines acquired from the government. Judging by the available CDC data, most states used only around 50 percent of received jabs with few notable exceptions. West Virginia used up 204,000 out of a total 243,000 shots available whereas California administered only 2.3 million jabs out of a possible 4.9 million - less than half its stockpile.
This drastic difference between the states' performance in distributing vaccines stems from differences in how they organise it, according to Dr Sanjay Mishra, a Staff Scientist at the Vanderbilt University Medical Centre in Nashville, Tennessee. He said that although some states used every resource available, including the National Guard - as seen in West Virginia - others relied only on distribution via local pharmacies. This, along with the discrepancies in states' population, resulted in the inconsistencies in local authorities' performance in inoculating the population, the scientist suggests.
"Sparsely populated states such as North Dakota, South Dakota and West Virginia have outperformed others by administering nearly all supply of first vaccines. West Virginia is even expected to be done inoculating nursing care residents with both doses by the end of January," Mishra says.
US Infrastructure Was Not Ready for Such Campaign
The fact that more highly populated states such as California lag behind in distribution of the vaccine only highlights the fact that the logistics ended up being one of the biggest challenges for the vaccination campaign in the US, Dr Mishra says.
However, the problem might be broader and may affect the entire country. The fact that states request new vaccine batches after not using their entire stock suggests the existence of a deeper problem with the US infrastructure, which was simply not ready to handle the ambitious vaccination campaign, Rutschman suggests.
"The US still does not have a vaccine distribution infrastructure that can accommodate the type of vaccine rollout necessary to respond to a large public health crisis. So you see states asking for more vaccine (which they need) while sometimes failing to administer all the doses they have," she adds.
The practice of holding back half of delivered vaccines was in effect throughout December to have enough medicine for the second shots both Moderna and Pfizer jabs require for forming the immunity. However, this approach was rescinded by the Trump administration almost two weeks ago and yet the situation hasn't changed in many states. In addition, some of them had less than 50 percent of received vaccines used up, but were still requesting more.
This issue might be linked to the fact that the two vaccines approved in the US demand special conditions for their storage, which is not helping the situation with botched logistics, Rutschman says. Pfizer/BioNTech vaccine requires a strict temperature regime ranging between −80 and −60 Celsius (−112 and −76 °F) for storage, whereas Moderna's jab needs a temperature range between -25 and -15 Celsius (-13 and 5°F). Several shipments of these vaccines have already been thrown out because storage rules have been broken during and after transportation.
What Can The Biden Administration Do About It?
The administration of the Democrat promised that in its first 100 days 100 million Americans will be inoculated. However, that goal can hardly serve as a benchmark of the efficiency of Biden's policy – the rate of vaccinations had practically reached a million per day in the past days of Trump's administration and its much-criticised Operation Warp Speed. Some media have already called on Biden to boost his goal to 200 million inoculations over first 100 days since the previous landmark was practically assured by his predecessor.
But what can the Democrat do to improve vaccination rates further? His seven-point plan for public health and the economy vaguely described efforts to provide every American with COVID-19 vaccine free of charge and invest some $25 billion in its manufacturing and distribution, but was short on detail.

The new administration intends to use the Federal Emergency Management Agency (FEMA) to erect community vaccination centres and launch a pharmacy programme to make the medicine available in more places across the country, Mishra suggests.
"This will expand the national pool of vaccinators, and will provide alternate to the poor performing states’ distribution system", the Vanderbilt University scientist explains.
Whether Pfizer and the federal logistics infrastructure will be able to keep up with such an ambitious task after causing vaccine shortages in some states over the past month and a half, remains to be seen.
Another issue that the Biden administration is likely to face is persisting high levels of vaccine hesitancy in the country regarding the coronavirus jab. The latest national poll conducted by Gallup International showed that only 46 percent of Americans were ready to take the jab at the beginning of January as soon as the opportunity presents itself. Although the number of those who were ready to get vaccinated on day one grew noticeably from the middle of 2020, the issue persists. A similar hesitancy is seen even among healthcare workers, and the issue might become more problematic in the future, Rutschman points out. The Democrat's team has so far not indicated how it intends to deal with this challenge in the near future.