https://sputnikglobe.com/20211230/covid-19-omicron-patients-spend-less-time-in-hospital--and-immune-cells-target-mutant-1091923075.html
COVID-19 Omicron Patients Spend Less Time in Hospital — And Immune Cells Target Mutant
COVID-19 Omicron Patients Spend Less Time in Hospital — And Immune Cells Target Mutant
Sputnik International
The Omicron variant of COVID-19 has spread rapidly across the globe in now more than a month, accounting for over 90 per cent of new infections in some... 30.12.2021, Sputnik International
2021-12-30T22:01+0000
2021-12-30T22:01+0000
2023-05-28T15:17+0000
omicron covid strain
coronavirus
covid-19
national health service (nhs)
immune system
pretoria
britain
great britain
vaccination
immunity
https://cdn1.img.sputnikglobe.com/img/07e4/0a/07/1080689598_0:0:3641:2048_1920x0_80_0_0_024d4c10fcd4ac387333afe1e69539b2.png
New data confirm that patients with the Omicron variant have shorter stays in hospital — and that the immune system recognises the new mutant.An article in The Spectator on Thursday reported on data made available to the British government's Scientific Advisory Group for Emergencies (SAGE) committee on December 22 — and seen by the magazine. It showed that that the average hospital stay for COVID patients had been cut radically since December 1 compared to the third wave of the virus in early to mid-2021.Admission times were down from four days to three for under-50s, around 6.5 days to 4.5 for those aged 50 to 69, from eight days to less than five for those in their 70s and almost 12 days to five for over-80s.The first case of the new variant was identified in England on November 27. It has since rapidly become dominant, accounting for 94 per cent of new cases according to the UK Health Security Agency.While daily case numbers have soared to record highs this week, the mortality rate has tumbled. The Scientific Pandemic Influenza Group on Modelling (SPI-M) wrote on December 23 that such a trend would give a much-needed respite to the National Health Service (NHS). The data supports a December 4 study from South Africa's Gauteng province, where Omicron was first identified, showing a three-fold cut in hospital stays."A significant early finding in this analysis is the much shorter average length of stay of 2.8 days for SARS-CoV-2 positive patients admitted to the COVID wards over the last two weeks compared to an average length of stay of 8.5 days for the past 18 months," the team of South African scientists and doctors said.On Tuesday, government scientific advisor Professor Sir John Bell backed the South African findings, saying Omicron was "not the same disease we were seeing a year ago"."The horrific scenes that we saw a year ago of intensive care units being full, lots of people dying prematurely, that is now history," Bell said. "I think we should be reassured that that’s likely to continue".Immune DefencesMeanwhile, a study of South African patients by a team of virologists, immunologists and medical scientists at the University of Cape Town found that while Omicron is able to evade antibodies against other variants, the body's white blood cells can still recognise and fight it.Their findings raise hopes that the widespread immunity built up in the population after two years of the pandemic will protect it from the new variant.The team confirmed that the 32 mutations to the Omicron variant's spike proteins — structures on the viral particle's protein coat that allow it to infect human cells — meant antibodies produced by vaccination or infection with other viruses could no longer lock onto it.But the authors found that "70-80 per cent of the CD4 and CD8 T cell response to spike was maintained across study groups".CD8 T cells fight infections by recognizing and destroying infected cells of the body — stopping them from acting as 'factories' for copies of the virus. They also attack cancer cells. The roving CD8 cells adapt to specific infections with T-cell receptors on their surface that recognise tell-tale antigens — surface proteins — in the outer membranes of infected cells. The CD4 or T helper cells play a key role in detecting infected cells and guiding the CD8 cells to destroy them, while also aiding the B cells of the immune system to produce antibodies tailored to the new pathogen.
https://sputnikglobe.com/20211228/from-pandemic-plague-to-seasonal-sniffle-how-viruses-mutate-into-milder-strains-to-survive-1091859984.html
pretoria
britain
great britain
cape town
south africa
united kingdom (uk)
Sputnik International
feedback@sputniknews.com
+74956456601
MIA „Rossiya Segodnya“
2021
James Tweedie
https://cdn1.img.sputnikglobe.com/img/07e4/08/1c/1080307270_0:3:397:400_100x100_80_0_0_7777393b9b18802f2e3c5eaa9cbcc612.png
James Tweedie
https://cdn1.img.sputnikglobe.com/img/07e4/08/1c/1080307270_0:3:397:400_100x100_80_0_0_7777393b9b18802f2e3c5eaa9cbcc612.png
News
en_EN
Sputnik International
feedback@sputniknews.com
+74956456601
MIA „Rossiya Segodnya“
Sputnik International
feedback@sputniknews.com
+74956456601
MIA „Rossiya Segodnya“
James Tweedie
https://cdn1.img.sputnikglobe.com/img/07e4/08/1c/1080307270_0:3:397:400_100x100_80_0_0_7777393b9b18802f2e3c5eaa9cbcc612.png
coronavirus, covid-19, national health service (nhs), immune system, pretoria, britain, great britain, vaccination, immunity, vaccines, cape town, south africa, united kingdom (uk)
coronavirus, covid-19, national health service (nhs), immune system, pretoria, britain, great britain, vaccination, immunity, vaccines, cape town, south africa, united kingdom (uk)
COVID-19 Omicron Patients Spend Less Time in Hospital — And Immune Cells Target Mutant
22:01 GMT 30.12.2021 (Updated: 15:17 GMT 28.05.2023) The Omicron variant of COVID-19 has spread rapidly across the globe in now more than a month, accounting for over 90 per cent of new infections in some countries and regions. But evidence is increasingly emerging that it is far less harmful than previous mutations of the pandemic virus.
New data confirm that patients with the Omicron variant have shorter stays in hospital — and that the immune system recognises the new mutant.
An article in
The Spectator on Thursday reported on data made available to the British government's Scientific Advisory Group for Emergencies (SAGE) committee on December 22 — and seen by the magazine.
It showed that that the average hospital stay for COVID patients had been cut radically since December 1 compared to the third wave of the virus in early to mid-2021.
Admission times were down from four days to three for under-50s, around 6.5 days to 4.5 for those aged 50 to 69, from eight days to less than five for those in their 70s and almost 12 days to five for over-80s.
The first case of the new variant was identified in England on November 27. It has since rapidly become dominant, accounting for 94 per cent of new cases according to the
UK Health Security Agency.
While daily case numbers have soared to
record highs this week, the mortality rate has tumbled.
The Scientific Pandemic Influenza Group on Modelling (SPI-M) wrote on December 23 that such a trend would give a much-needed respite to the National Health Service (NHS).
"A reduced length of stay would allow more capacity within hospitals to manage this, and, to a first approximation, this would scale linearly with the change, i.e. halving the length of stay would permit double the admissions," it said.
The data supports a
December 4 study from South Africa's Gauteng province, where Omicron was first identified, showing a three-fold cut in hospital stays.
"A significant early finding in this analysis is the much shorter average length of stay of 2.8 days for SARS-CoV-2 positive patients admitted to the COVID wards over the last two weeks compared to an average length of stay of 8.5 days for the past 18 months," the team of South African scientists and doctors said.
On Tuesday, government scientific advisor Professor Sir John Bell
backed the South African findings, saying Omicron was "not the same disease we were seeing a year ago".
"The horrific scenes that we saw a year ago of intensive care units being full, lots of people dying prematurely, that is now history," Bell said. "I think we should be reassured that that’s likely to continue".
28 December 2021, 18:42 GMT
Meanwhile,
a study of South African patients by a team of virologists, immunologists and medical scientists at the University of Cape Town found that while Omicron is able to evade antibodies against other variants, the body's white blood cells can still recognise and fight it.
Their findings raise hopes that the widespread immunity built up in the population after two years of the pandemic will protect it from the new variant.
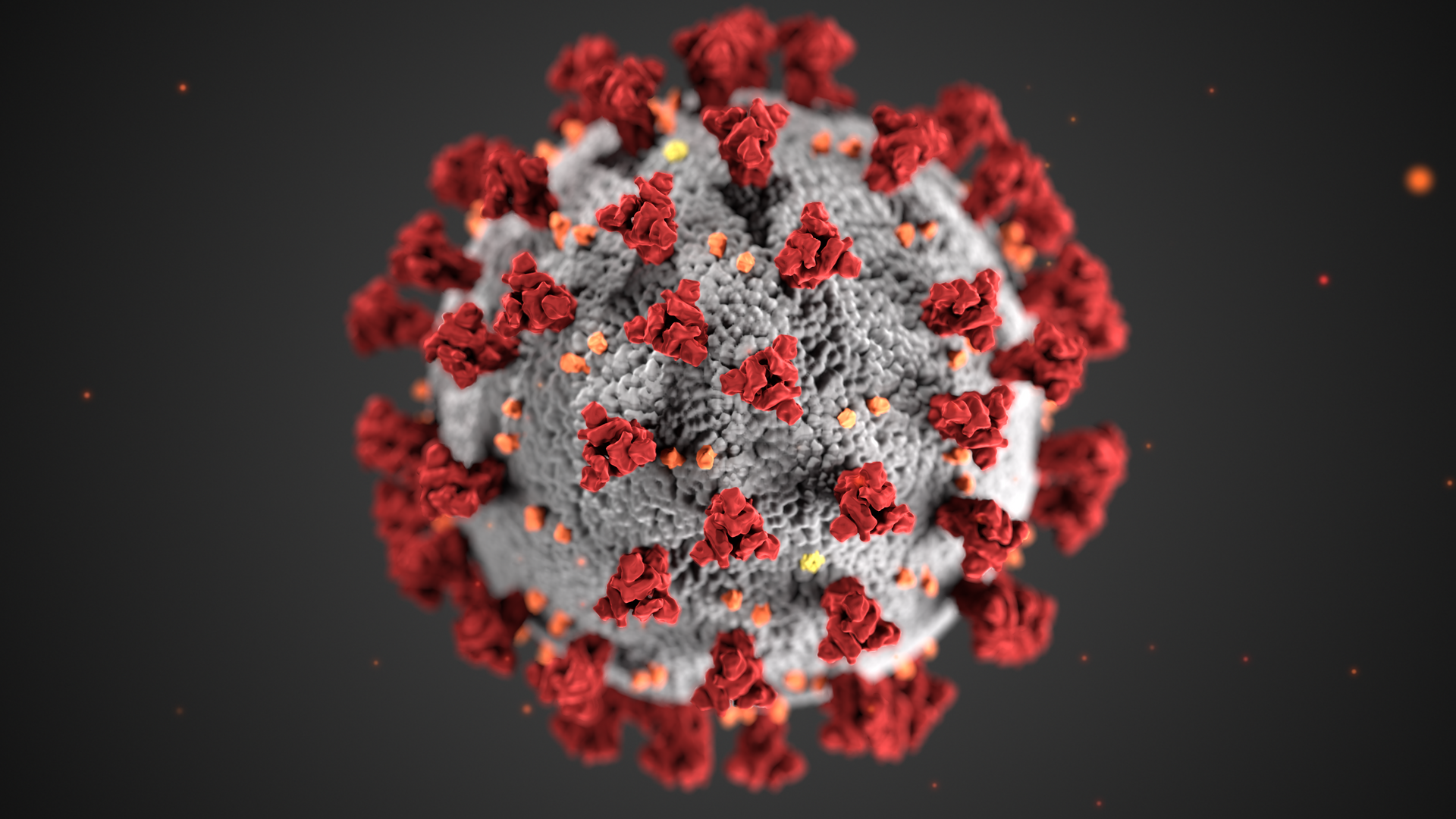
The team confirmed that the 32 mutations to the Omicron variant's spike proteins — structures on the viral particle's protein coat that allow it to infect human cells — meant antibodies produced by vaccination or infection with other viruses could no longer lock onto it.
But the authors found that "70-80 per cent of the CD4 and CD8 T cell response to spike was maintained across study groups".
"Moreover, the magnitude of Omicron cross-reactive T cells was similar to that of the Beta and Delta variants, despite Omicron harbouring considerably more mutations," they wrote.
CD8 T cells fight infections by recognizing and destroying infected cells of the body — stopping them from acting as 'factories' for copies of the virus. They also attack cancer cells.
The roving CD8 cells adapt to specific infections with T-cell receptors on their surface that recognise tell-tale antigens — surface proteins — in the outer membranes of infected cells.
The CD4 or T helper cells play a key role in detecting infected cells and guiding the CD8 cells to destroy them, while also aiding the B cells of the immune system to produce antibodies tailored to the new pathogen.