https://sputnikglobe.com/20220623/drug-resistant-typhoid-fever-poses-risk-of-new-global-spread-study-says-1096605808.html
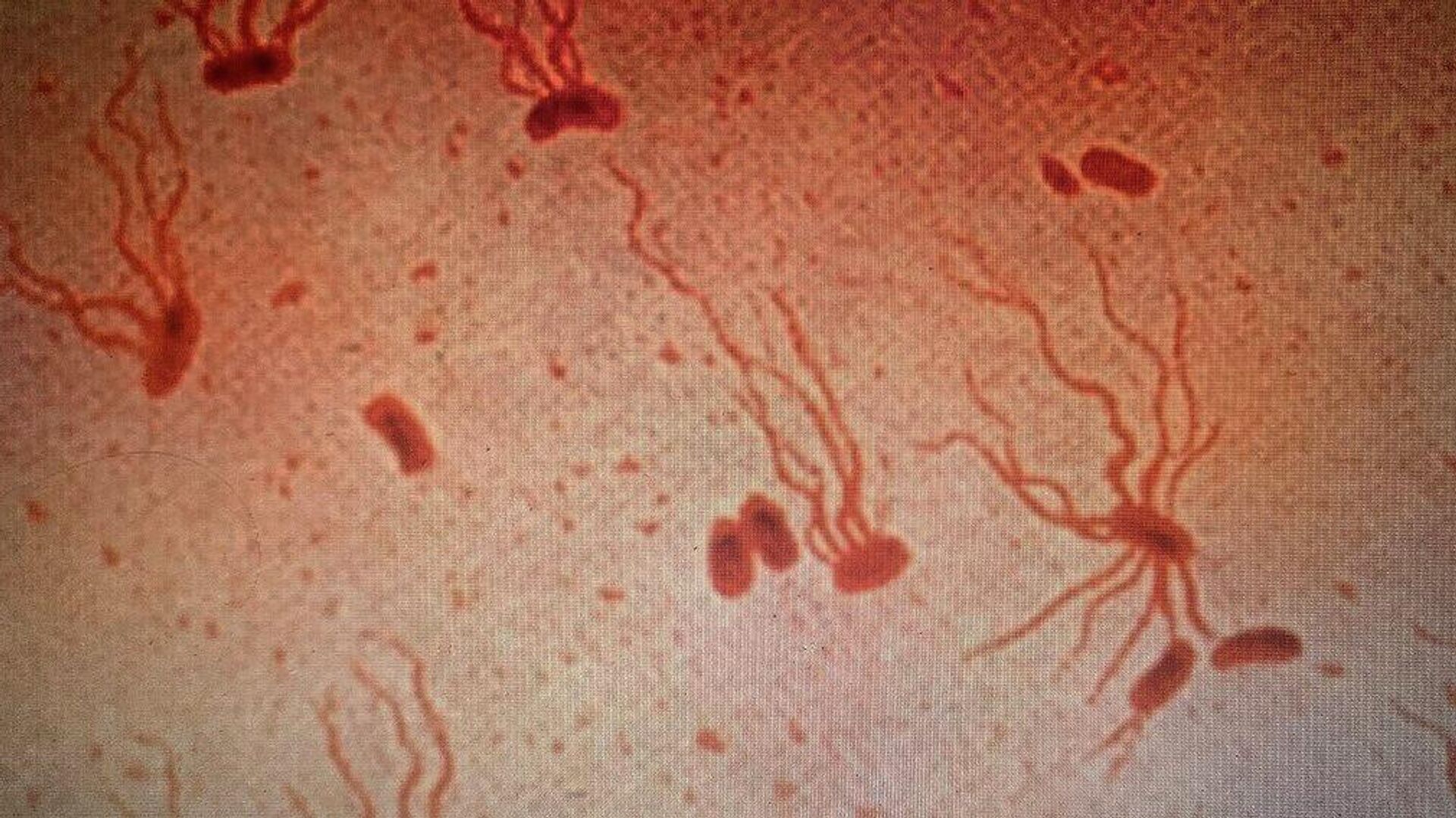
Drug-Resistant Typhoid Fever Poses Risk of New Global Spread, Study Says
Drug-Resistant Typhoid Fever Poses Risk of New Global Spread, Study Says
Sputnik International
A new medical study has found that the bacteria that causes typhoid fever is learning to adapt to the last major antibiotic still capable of treating it... 23.06.2022, Sputnik International
2022-06-23T20:24+0000
2022-06-23T20:24+0000
2022-06-23T20:22+0000
fever
study
antibiotics
typhoid fever
https://cdn1.img.sputnikglobe.com/img/07e6/06/17/1096606409_8:0:1018:568_1920x0_80_0_0_723037d1d7a7ddf114d4e0118c329e80.jpg
According to a study published in The Lancet Microbe on Tuesday, tests on several different strains of Salmonella enterica serovar Typhi (S Typhi) bacteria found mutations making them more resistant to the antibiotic azithromycin, and that those strains are rapidly replacing others.The samples were gathered in Nepal, Bangladesh, Pakistan, and India between 2014 and 2019.The find, the scientists say, “threatens the efficacy of all oral antimicrobials for typhoid treatment.”“At the same time, the fact resistant strains of S. Typhi have spread internationally so many times also underscores the need to view typhoid control, and antibiotic resistance more generally, as a global rather than local problem,” he added.The bacteria that causes typhoid is most commonly spread by consuming water contaminated with feces from another person already infected by the bacteria, although it can be spread by a variety of methods if sanitary practices are poor. It causes a severe enteric fever that without treatment can kill 20% of those infected, although treatment drops the death rate to between 1% and 4%.As such, the disease proliferates in parts of the world with poor sanitation, with several million cases being reported each year in South Asia and Africa, but also several hundred to several thousand in the United States as well.Antibiotics have been used to treat infection since the 1940s, although the emergence of resistant strains was observed almost immediately. A vaccine is capable of preventing up to 90% of infections within two years of being administered, although its effectiveness steadily wanes.
Sputnik International
feedback@sputniknews.com
+74956456601
MIA „Rossiya Segodnya“
2022
Sputnik International
feedback@sputniknews.com
+74956456601
MIA „Rossiya Segodnya“
News
en_EN
Sputnik International
feedback@sputniknews.com
+74956456601
MIA „Rossiya Segodnya“
Sputnik International
feedback@sputniknews.com
+74956456601
MIA „Rossiya Segodnya“
fever, study, antibiotics, typhoid fever
fever, study, antibiotics, typhoid fever
Drug-Resistant Typhoid Fever Poses Risk of New Global Spread, Study Says
A new medical study has found that the bacteria that causes typhoid fever is learning to adapt to the last major antibiotic still capable of treating it, meaning stopping the spread of the deadly disease will become much harder.
According to a study published in
The Lancet Microbe on Tuesday, tests on several different strains of Salmonella enterica serovar Typhi (S Typhi) bacteria found mutations making them more resistant to the antibiotic azithromycin, and that those strains are rapidly replacing others.
The samples were gathered in Nepal, Bangladesh, Pakistan, and India between 2014 and 2019.
The find, the scientists say, “threatens the efficacy of all oral antimicrobials for typhoid treatment.”
"The speed at which highly-resistant strains of S. Typhi have emerged and spread in recent years is a real cause for concern, and highlights the need to urgently expand prevention measures, particularly in countries at greatest risk," Stanford University infectious disease specialist Jason Andrews said in a
Wednesday media release.
“At the same time, the fact resistant strains of S. Typhi have spread internationally so many times also underscores the need to view typhoid control, and antibiotic resistance more generally, as a global rather than local problem,” he added.
The bacteria that causes typhoid is most commonly spread by consuming water contaminated with feces from another person already infected by the bacteria, although it can be spread by a variety of methods if sanitary practices are poor. It causes a severe enteric fever that without treatment can kill 20% of those infected, although treatment drops the death rate to between 1% and 4%. As such, the disease proliferates in parts of the world with poor sanitation, with several million cases being reported each year in South Asia and Africa, but also several hundred to several thousand in the United States as well.
Antibiotics have been used to treat infection since the 1940s, although the emergence of resistant strains was
observed almost immediately. A vaccine is capable of preventing up to 90% of infections within two years of being administered, although its effectiveness steadily wanes.